The concept of preventive healthcare has evolved dramatically over the past decade. While annual checkups and cancer screenings remain foundational, a new frontier has emerged that addresses the gradual decline in vital hormones that affects virtually everyone as they age.
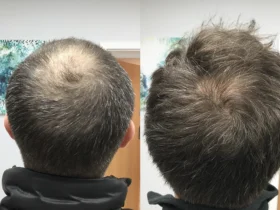
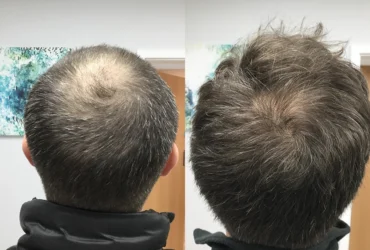
Rather than waiting for symptoms to become debilitating, forward thinking patients and physicians are now exploring how treatments like Men’s hormone optimization therapy can maintain vitality, prevent chronic disease, and enhance quality of life decades before traditional medical intervention would typically begin. This shift represents a fundamental rethinking of when and how we address age related decline.
The science supporting hormone optimization as preventive medicine has reached a critical mass that can no longer be ignored by mainstream healthcare. What was once dismissed as anti aging vanity has proven to be legitimate disease prevention backed by rigorous clinical research.
Understanding the Hormone Decline Timeline
Hormones function as chemical messengers that regulate virtually every bodily system, from metabolism and immune function to cognitive performance and emotional wellbeing. The decline in key hormones doesn’t happen suddenly but follows predictable patterns that begin much earlier than most people realize.
Testosterone levels in men peak in the late teens to early twenties, then decline approximately 1% to 2% per year after age 30. By age 50, many men have testosterone levels 30% to 40% lower than their peak, even though this remains technically within the broad “normal” range established by laboratory reference values.
Growth hormone secretion drops even more dramatically, decreasing by roughly 14% per decade after age 20. By age 60, growth hormone production is typically less than half of youthful levels. Thyroid function often becomes sluggish with age, and DHEA, sometimes called the “mother hormone” because it serves as a precursor to other hormones, declines steadily throughout adulthood.
Women experience their own complex hormonal transitions, with estrogen and progesterone fluctuating through perimenopause before dropping sharply at menopause. These changes affect not just reproductive function but bone density, cardiovascular health, cognitive function, and metabolic regulation.
| Hormone | Peak Age | Age 40 Levels | Age 60 Levels | Primary Functions Affected |
| Testosterone (Men) | 18 to 25 | 80% to 90% of the peak | 50% to 70% of the peak | Muscle mass, bone density, libido, energy |
| Estrogen (Women) | 20 to 30 | 70% to 100% variable | 10% to 30% of the peak | Bone health, cardiovascular, and cognitive |
| Growth Hormone | 18 to 25 | 60% to 70% of the peak | 30% to 40% of the peak | Body composition, recovery, skin quality |
| DHEA | 20 to 30 | 60% to 80% of the peak | 20% to 40% of the peak | Energy, immune function, mood |
| Thyroid (T3/T4) | 20 to 40 | 90% to 100% normal | 70% to 90% normal | Metabolism, energy, temperature regulation |
The Preventive Healthcare Paradigm Shift
Traditional medicine has operated on a reactive model: wait until disease manifests, then treat symptoms. A person experiencing fatigue, weight gain, and low mood might receive antidepressants and lifestyle advice without anyone checking whether declining hormones underlie these complaints.
The preventive model flips this approach. By identifying and addressing hormonal insufficiency before it progresses to clinical disease, we can potentially prevent or delay conditions including osteoporosis, cardiovascular disease, sarcopenia (age related muscle loss), cognitive decline, and metabolic syndrome.
Research published in the Journal of Clinical Endocrinology & Metabolism found that men with low testosterone had a 33% higher risk of death over 18 years compared to men with normal levels. Studies have linked testosterone deficiency to increased cardiovascular disease risk, type 2 diabetes, and cognitive impairment.
Similarly, research on growth hormone deficiency in adults has documented increased cardiovascular risk, reduced bone density, unfavorable changes in body composition, and decreased quality of life. Addressing these deficiencies before they contribute to disease represents true preventive medicine.
The key distinction is that hormone optimization for prevention differs from treating hormone deficiency diseases. The latter addresses severe deficiency causing obvious symptoms, while the former seeks to maintain hormones at youthful functional levels to preserve health and vitality.
Who Benefits from Hormone Optimization
Not everyone requires hormone optimization therapy, but certain populations stand to benefit substantially. Men over 35 experiencing unexplained fatigue, decreased muscle mass despite exercise, reduced libido, difficulty concentrating, or mood changes should consider comprehensive hormone testing.
Women experiencing perimenopausal symptoms including irregular periods, hot flashes, sleep disturbances, mood swings, or vaginal dryness represent another key group. Rather than simply enduring these symptoms as inevitable aspects of aging, bioidentical hormone replacement can dramatically improve quality of life while protecting bone density and cardiovascular health.
Athletes and highly active individuals may notice performance declines earlier than sedentary people because they’re more attuned to their bodies’ capabilities. Someone who’s always maintained a rigorous workout routine will notice when recovery slows, strength plateaus despite consistent training, or endurance diminishes.
People with strong family histories of osteoporosis, cardiovascular disease, or dementia might benefit from hormone optimization as part of a comprehensive prevention strategy. While hormones alone cannot eliminate genetic risk, maintaining optimal levels addresses modifiable risk factors.
Comprehensive Testing Beyond Basic Panels
The foundation of any hormone optimization program is thorough testing, but standard annual checkups rarely include comprehensive hormone panels. Basic lab work might check total testosterone in men or TSH for thyroid function, but these limited snapshots miss crucial information.
Optimal hormone assessment includes total and free testosterone (the biologically active form), estradiol, DHEA sulfate, complete thyroid panel including T3 and T4, cortisol, vitamin D (technically a hormone), and potentially growth hormone markers like IGF1. For men, assessing estradiol is particularly important because testosterone can convert to estrogen, causing its own set of problems.
Testing should ideally occur in the morning when many hormones peak, and results should be evaluated in clinical context rather than simply checking whether values fall within broad reference ranges. A 45 year old man with testosterone of 350 ng/dL is technically “normal” by lab standards (which might range from 300 to 1000 ng/dL) but is functioning at levels typical of a much older man.
Repeat testing establishes baselines and tracks response to interventions. Hormone levels fluctuate, so single measurements provide limited information compared to monitoring trends over time.
Treatment Modalities and Delivery Methods
Hormone optimization employs various delivery methods, each with distinct advantages and considerations. Testosterone replacement for men includes injections (weekly or biweekly), topical gels or creams (daily application), patches, and subcutaneous pellets (inserted every three to six months).
Injections provide reliable dosing and are generally most cost-effective, though some men dislike needles or experience peaks and valleys between doses. Topical preparations offer convenience but require careful application to avoid transferring hormone to partners or children. Pellets provide steady hormone release but require minor office procedures for insertion.
Women’s hormone replacement typically uses bioidentical estradiol and progesterone in forms including patches, creams, oral medications, or pellets. The route of administration matters significantly; transdermal estrogen avoids the first pass liver metabolism of oral preparations, potentially reducing risks.
Thyroid optimization might involve T4-only preparations (levothyroxine), combination T4/T3 medications, or desiccated thyroid extract, depending on individual needs. Growth hormone therapy remains expensive and is typically reserved for documented deficiency rather than optimization, though peptides that stimulate natural growth hormone production offer alternatives.
DHEA supplementation is straightforward as it’s available over the counter, though medical supervision ensures appropriate dosing and monitoring.
Monitoring and Adjusting Protocols
Hormone optimization is not a set it and forget it intervention. Responsible programs include regular follow up, repeated lab testing, and dosage adjustments based on both objective measurements and subjective response.
Initial monitoring typically occurs every three months during the first year, allowing providers to fine tune dosages and identify any adverse effects early. Once stable, many patients transition to semiannual or annual monitoring depending on their specific protocols.
Important safety parameters include hemoglobin and hematocrit (testosterone can increase red blood cell production), prostate specific antigen in men, lipid panels, liver enzymes, and bone density scans for women on estrogen replacement.
The goal is achieving hormone levels consistent with healthy younger adults while monitoring for potential side effects. This requires physicians knowledgeable about optimal ranges rather than simply normalizing lab values into broad reference ranges designed to identify disease rather than optimize function.
Addressing Safety Concerns and Misconceptions
Hormone therapy has faced controversy, partly due to poorly designed studies and misunderstanding of research findings. The Women’s Health Initiative study published in 2002 raised concerns about hormone replacement therapy, leading millions of women to discontinue treatment despite the study’s significant limitations.
Subsequent analysis revealed the increased risks applied primarily to older women (average age 63) starting synthetic hormones years after menopause, not younger women using bioidentical hormones around the time of menopause. The risk benefit calculation differs dramatically based on age, timing, hormone type, and delivery method.
For men, concerns about testosterone therapy and cardiovascular risk have been debated extensively. More recent large scale studies have actually suggested cardiovascular benefits in men with documented low testosterone who receive appropriate treatment, while poorly monitored therapy or use of testosterone in men with normal levels might carry risks.
The safety of hormone optimization depends critically on proper patient selection, appropriate dosing, careful monitoring, and using bioidentical hormones via optimal delivery methods. It’s neither universally safe nor universally dangerous; context determines outcomes.
Integration with Lifestyle Optimization
Hormone therapy should never serve as a substitute for foundational health practices. The most effective approach combines hormone optimization with nutrition, exercise, sleep, and stress management.
Resistance training amplifies the benefits of testosterone optimization by building muscle mass and strength. Adequate protein intake supports lean tissue maintenance. Quality sleep is when the body produces growth hormone naturally, so sleep optimization magnifies the benefits of any growth hormone supporting interventions.
Stress management matters because chronic elevation of cortisol antagonizes other hormones and contributes to metabolic dysfunction. Meditation, appropriate exercise (not excessive training that drives cortisol up), and work life balance all support hormonal health.
Some patients discover through comprehensive evaluation that lifestyle factors are substantially contributing to their hormone issues. Obesity suppresses testosterone production in men. Extreme calorie restriction or excessive exercise can disrupt women’s hormonal cycles. Addressing these factors might reduce or eliminate the need for hormone therapy.
The Economic Case for Prevention
From a healthcare economics perspective, hormone optimization as preventive medicine could potentially reduce long term costs by preventing or delaying expensive chronic diseases. Osteoporosis leads to fractures requiring surgery and rehabilitation. Cardiovascular disease generates enormous treatment costs. Cognitive decline and dementia create massive caregiving expenses.
If maintaining optimal hormone levels delays the onset of these conditions by even a few years, the cost savings could dwarf the expense of hormone therapy and monitoring. A patient spending $2,000 annually on hormone optimization who avoids a $75,000 hip fracture surgery or delays nursing home placement has achieved substantial economic benefit alongside the personal health gains.
Insurance coverage for hormone optimization remains inconsistent, with some plans covering treatment for diagnosed deficiency but not preventive optimization. This may shift as evidence accumulates and preventive medicine gains broader acceptance, but currently many patients pay out of pocket.
Looking Toward the Future
The field of hormone optimization continues evolving rapidly. Ongoing research is identifying optimal target levels for different populations, refining delivery methods, and developing new biomarkers for monitoring.
Personalized medicine approaches using genetic testing may eventually allow prediction of who will benefit most from specific interventions. Advanced imaging and functional testing could provide earlier detection of the subtle changes that precede clinical disease.
As the population ages and healthcare systems strain under the burden of chronic disease, the appeal of interventions that maintain vitality and prevent decline will only grow. Hormone optimization sits at the intersection of extending healthspan (years lived in good health) rather than merely lifespan.
The question facing medicine is whether we’ll embrace this preventive approach proactively or continue defaulting to reactive treatment of established disease. For individuals, the choice is whether to accept gradual decline as inevitable or to explore interventions that might preserve the energy, strength, and mental clarity that make life worth living well into older age.
Hormone optimization will never be a magic bullet, and it’s certainly not appropriate for everyone. But for well selected patients under competent medical supervision, it represents a legitimate tool in the growing arsenal of preventive healthcare strategies that address aging as a modifiable process rather than an immutable fate.